A ‘Cool’ Way to Transport or Not?
Since their successful conception in 1967 by Dr. Christiaan Barnard, heart transplants have been a staple in the transplant world. They have provided many individuals with end stage cardiomyopathy (weakening of the heart muscles), heart valve disease, coronary artery disease, or other cardiovascular diseases a second chance at life. However, even as medical technology rapidly progressed over the years, one part of the heart transplant procedure remained relatively the same: the process of transporting a donor heart.
Traditionally, once a donor heart becomes available, it is removed from the donor’s body, sealed in a plastic bag, and then placed in an ice cooler. The cooler is then transported to the hospital where the heart transplant surgery will occur. While this might be the most common method for transportation, it is definitely not the most effective. On average, 8 out of 10 donor hearts don’t make it to transplant surgery. This can be due to the limited amount of time a heart can remain outside of the body, formally known as ischemic time. A heart can ideally last outside of the body for 4-6 hours. If the time goes longer than that, then the ice surrounding the heart can begin to cause irreversible damage to the heart cells, leaving it unable to be restarted. Because of this short transport time period and possibility of cellular damage, it’s very difficult to transport a heart successfully, even if the donor is a perfect match. In 2017 alone, only 3,244 hearts were transplanted when an estimated 100,000 patients needed a new heart.
However, a new solution to this problem is currently in the works thanks to a company called Transmedics.
Transmedics: Heart in a Box
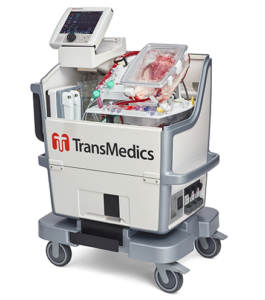
In the early 2010s, Transmedics brought a new method of donor heart transportation to the table, and it came in the form of a mechanical box. Heart in a Box or the Organ Care System (OSC) Heart served a radical idea: what if we could keep a heart beating during transport?
And they accomplished just that! Once a donor’s heart becomes available for transport, it is placed inside the (OSC) Heart, where doctors will hook tubes into the aorta (the main artery that pumps oxygenated blood to the rest of the body) and the pulmonary vein (which transfers oxygenated blood from the lungs to the heart). These tubes are used to pump oxygenated blood sourced from the donor through the heart by mimicking the changes in pressures inside the left ventricle and left atria. From this process, the heart receives the necessary nutrients and oxygen needed to function properly, meaning that it can basically be kept alive outside of the body thus eliminating ischemic time. The OSC even comes with a portable tablet that monitors the vitals of the heart (such as rhythm and heartbeat) and allows for direct changes to be made to pump flow rate or nutrient levels to keep the heart functioning properly throughout the transport process.
With the heart kept alive and beating, the time limit for transport is vastly increased. Current trials have shown that with OSC, donor hearts can remain viable for up to 12 hours, double what could be achieved with the cooler! With the heart being constantly monitored to maintain proper function instead of being iced and not beating, it also eases the process of restarting the heart in the recipient’s body. These changes could mean huge advancements in the number of patients that successfully receive a donor heart for transplant. The OSC Heart is still undergoing FDA clinical trials to prove its safety and benefit to heart transplant recipients before it becomes a wide scale method of transport, but so far many transplants that have occurred with the device have been successful. Transmedics is even branching out to using similar OSC for other organ transplants, such as lungs and kidneys. As of now, we’re on track for a brighter future for transportation of donor organs.
The Heart Beats On
The story of Transmedics reminds us of a valuable lesson: just because a medical procedure or device is widespread doesn’t mean that it is most effective. Current methodology needs to be questioned to look for ways of improvement. Nothing is perfect. Sometimes creativity and innovation are needed to cause a paradigm shift that can completely change how the world handles a medical issue. Never stop looking for scientific improvement! You never know if your idea might end up saving someone’s life.
Citations
Breining, Greg. “Heart in a Box.” Medical School – University of Minnesota, 28 Mar. 2017, med.umn.edu/news-events/medical-bulletin/heart-box.
Breining, Greg. “Transplant Transport.” Legacy, 11 Sept. 2018, discoverymag.umn.edu/stories/transplant-transport.
“Heart Transplant.” Mayo Clinic, Mayo Foundation for Medical Education and Research, 16 Nov. 2019, www.mayoclinic.org/tests-procedures/heart-transplant/about/pac-20384750.
“OCS Heart for Patients and Families.” Transmedics, www.transmedics.com/ocs-heart/.